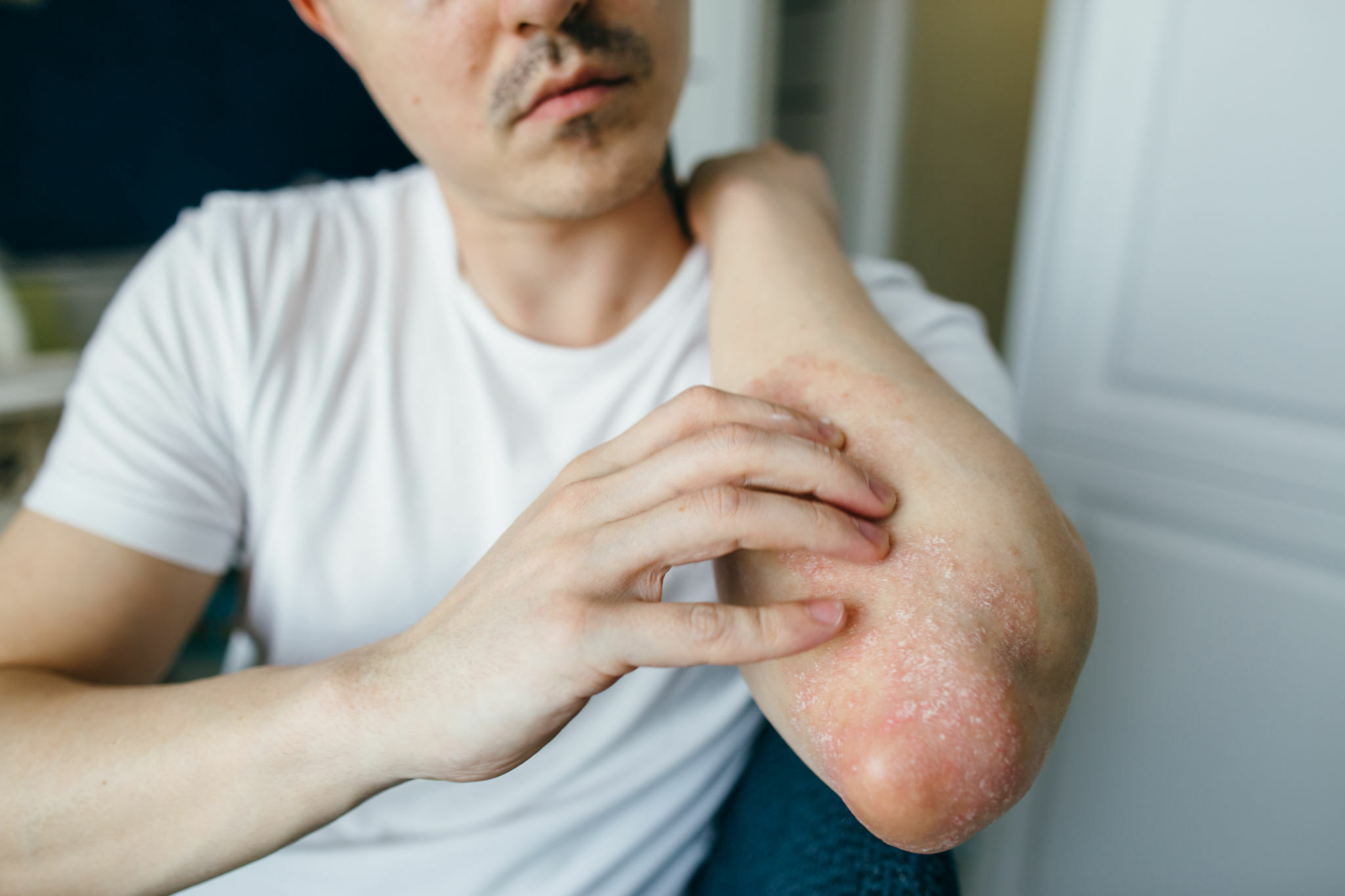
How to cure fungal infection on skin
Fungal skin infections, fungal dermatitis, cutaneous mycoses, and tinea are extremely common contagious conditions. Various species of fungi, such as yeast and mold, cause them. Approximately 25% of the global population is affected by superficial fungal skin infections at any time. These infections often result in irritating symptoms on the skin, including itching, redness, scaling, cracking, and rash. While they can occur anywhere on the body, fungal skin infections frequently develop in warm areas with folds of skin where moisture accumulates, such as between the toes, in the groin, and under the breasts.
The part of the body affected typically categorizes fungal skin infections. Some of the most common types are athlete’s foot, jock itch, ringworm, and yeast infections. The underlying causes are similar across the various types. They occur when the fungus is overgrowth on the skin, often encouraged by warm, humid conditions. Risk factors include excessive sweating, wearing tight clothing that doesn’t allow the skin to breathe, a weak immune system, and diabetes.
While fungal skin infections can be annoying and uncomfortable, they are treatable with over-the-counter topical antifungal creams, prescription medications, and home remedies. Proper hygiene and preventing moisture buildup on the skin can also help avoid recurrent infections. If basic treatments are ineffective, seeing a doctor to confirm the diagnosis and explore other options is important.
Symptoms
Fungal skin infections can cause a variety of symptoms affecting the skin. The most common symptoms include:
-
Itching, redness, and rash in the affected area. The rash may consist of small red bumps or patches.
-
We are scaling, cracking, or peeling of the skin. The skin may have a dry, flaky appearance.
-
Itching and rash often occur in skin folds where moisture collects, such as between the toes or fingers, under the breasts, groin, or arms.
-
Additional symptoms may include burning, stinging, or discomfort on the skin.
The appearance and location of the rash depend on the type of fungal infection. For example, an athlete’s foot causes scaling and cracking between the toes. Ringworm often causes a red, circular rash. Yeast infections lead to itching in moist areas like the genitals and skin folds.
Causes
Fungal skin infections are caused by an overgrowth of fungi like yeast and mold on the skin. The most common culprits are the fungi Trichophyton, Epidermophyton, and Candida. When conditions are right, these fungi can multiply rapidly on the skin.
Several factors create an environment that enables fungal overgrowth:
-
Humidity and Moisture – Fungi thrive in warm, moist environments. Perspiration, damp clothing, and wet surfaces foster fungal growth. Tight clothing that traps moisture is problematic.
-
Weakened Immune System – Fungi are opportunistic organisms that can exploit lowered immunity to overpopulate skin. Medical conditions like diabetes or immune deficiencies raise susceptibility.
-
Skin Irritation – Any damage to the outer skin layer enables easier fungal invasion. Cuts, burns, eczema, or abrasions provide an entry point.
-
Poor Hygiene – Not properly washing and drying skin or wearing unlaundered clothing leads to fungal buildup. Shared showers, gym equipment, and clothing also transmit fungi.
Controlling moisture, boosting immunity, and practicing good hygiene help prevent fungal overgrowth on the skin. Keeping skin clean, dry, and healthy can stop infections before they start.
Risk Factors
Certain groups are more prone to developing fungal skin infections. Risk factors include:
-
Athletes: Sweating and humid locker room environments create ideal conditions for fungi to thrive in places like the feet. Using public showers goes hand-in-hand with developing an athlete’s foot. Wearing tight shoes and socks that don’t breathe adds to the problem.
-
Obesity: Overweight individuals are more likely to develop skin fold fungal infections. Excess skin rubbing together harbors warmth and moisture. Yeast infections are particularly common in obese patients.
-
Diabetes: High blood sugar allows fungi to grow more rapidly. People with diabetes are susceptible to all types of fungal skin infections. Keeping blood sugar under control is key.
-
Antibiotics & Corticosteroids: Medications that suppress the immune system reduce the body’s defenses against fungal overgrowth. Fungal skin issues often arise after taking a course of antibiotics or steroids.
-
Hot & Humid Climates: Fungi thrive in environments where heat and humidity predominate. Tropical areas see high rates of skin fungal infections. Prevention focuses on keeping the skin clean and dry.
Diagnosis
Fungal skin infections are typically diagnosed through a visual exam and lab tests. During a physical exam, the doctor will look for signs of the infection, such as redness, scaling, cracking, itching, and rashes. They may also ask questions about symptoms and possible risk factors.
The doctor may examine a skin scraping or nail clipping under a microscope to confirm the diagnosis. A potassium hydroxide (KOH) solution is applied to the sample to help identify fungal elements. The skin cells are also checked for signs of fungal overgrowth like hyphae and spores. This microscopic examination can identify if a fungal infection is present and what specific type it may be.
Visual inspection combined with skin scraping allows dermatologists and doctors to diagnose fungal skin infections definitively. Once diagnosed, appropriate antifungal treatment can begin.
Types of Fungal Skin Infections
Fungal skin infections come in several common types:
Athlete’s Foot
An athlete’s foot, known as tinea pedis, is a contagious fungal infection that often occurs between the toes. It causes redness, scaly skin, blisters, and itching on the feet, especially between the toes and on the soles. It thrives in warm, moist environments like pools, showers, and locker rooms. It’s named “athlete’s foot” since it frequently affects athletes who wear tight shoes and socks. Antifungal creams, sprays, or powders are effective treatments.
Jock Itch
Jock itch, known medically as tinea cruris, is a fungal infection of the groin area. It leads to an itchy, red, often ring-shaped rash in the skin folds around the inner thighs and genitals. It occurs more often in men and can be transmitted through contact with infected towels, clothing, or surfaces. Keeping the area dry and using antifungal creams or powders clears up most cases.
Ringworm
Despite its name, ringworm is not caused by worms but by fungal infection. Ringworm, or tinea corporis, causes ring-shaped, red, itchy patches on the skin. The telltale ring is from the center of the patch, clearing as it grows outward. Ringworm thrives on the scalp, feet, groin, and trunk. Oral and topical antifungals treat most cases while keeping skin clean and dry.
Yeast Infections
Yeast infections result from overgrowth of the Candida fungus on the skin or mucous membranes. Common fungal yeast infections include oral thrush, vaginal yeast infections, and diaper rash. Yeast thrives in warm, moist conditions. Yeast infections cause redness, irritation, discharge, and itching. Antifungal creams, ointments, or suppositories clear most yeast infections. Some may require prescription oral antifungals.
Athlete’s Foot
An athlete’s foot is a fungal skin infection that most commonly affects the feet. This condition gets its name because it frequently occurs in athletes and active individuals prone to sweating. However, anyone can develop an athlete’s foot.
This fungal infection leads to symptoms like itching, burning, and stinging on the feet. It often starts between the toes, causing the skin to become red and cracked. There may also be peeling, flaky skin on the soles and sides of the feet. Sometimes, the toenails can become thick, discolored, and detached from the nail bed.
Athlete’s foot thrives in the moist, warm environment of sweaty feet, especially when feet are confined in tight shoes and socks. Direct contact in communal showers or locker room floors can also spread the fungal spores. Proper hygiene, promptly drying the feet, and changing into clean, dry socks can help prevent and treat athlete’s foot. Over-the-counter antifungal creams and medicated foot powders are effective for mild infections. Prescription oral antifungals may be needed for severe or recurring cases.
Jock Itch
Jock itch, also known as tinea cruris, is a fungal infection of the groin area caused by dermatophytes. It mainly affects the inner thighs, groin, and buttocks.
The main symptom of jock itch is a red, flaky, itchy rash in the folds of skin in the groin. The affected area may also burn or sting, especially when sweating during exercise or sports. Jock itch can spread to the genitals and inner thighs if left untreated.
Some additional symptoms of jock itch include:
- Red, circular rash with elevated edges
- Peeling, cracking, or flaking skin
- Itching, burning sensation in the groin
- Rash worsens with friction from clothes
- Rash spreads to inner thighs and buttocks
Jock itch tends to affect people who sweat a lot in the groin area, such as athletes, particularly those who play sports that require tight clothing, like cyclists and runners. The warm, moist environment encourages overgrowth of the fungus.
Wearing tight, restrictive clothing and underwear can trap heat and moisture in the groin. Not drying properly after showering or swimming also raises the risk of developing a jock itch. It can spread through contact with contaminated items like clothing or towels.
Jock itch can usually be treated with over-the-counter antifungal creams, medicated powders, and improved hygiene practices. Keeping the area dry and changing out of damp clothes right after exercise can help clear up the infection and prevent recurrence.
Ringworm
Ringworm is a type of fungal infection that presents as a red, circular rash with a scaly, raised border. The name ringworm comes from the ring-like appearance of the rash. Despite the name, ringworm is not caused by a worm, but by a fungus.
Ringworm can develop anywhere on the body where fungal infections thrive, such as moist areas like the feet (athlete’s foot), groin (jock itch), and scalp. Ringworm commonly occurs in children, but anyone can get ringworm.
The ringworm fungus lives on the outer layer of the skin and spreads outward as it multiplies, forming the characteristic ring-shaped rash. As the fungus grows, the center of the ring often clears up, so the raised, scaly border is the most prominent feature.
Ringworm can be spread through direct skin-to-skin contact with an infected person or animal. Touching contaminated surfaces like shower floors or shared equipment can also spread ringworm. Symptoms usually appear 4-14 days after exposure.
Ringworm is contagious as long as the rash is untreated. Over-the-counter antifungal creams are effective in treating ringworm. Keeping the affected area clean and dry can help speed healing.
To prevent ringworm, avoid sharing towels or clothing with someone who has ringworm. Promptly treating ringworm helps stop the spread to other parts of the body or other people. With treatment, ringworm usually clears up within a few weeks.
Yeast Infections
Yeast infections are fungal infections caused by an overgrowth of the Candida fungus, a yeast that normally lives inside the body in small amounts. An overgrowth of Candida leads to infection.
The most common locations for yeast infections include the following:
-
Vaginal yeast infections (vaginal thrush) – Characterized by vaginal discharge, genital itching and burning. The discharge is often thick, white, and curd-like (resembling cottage cheese). Vaginal yeast infections are very common, affecting up to 75% of women at least once in their lifetime.
-
Oral thrush – A yeast infection of the mouth characterized by white lesions on the tongue, inner cheeks, and sometimes the roof of the mouth. Oral thrush is most commonly seen in infants, toddlers, and immunocompromised individuals.
-
Candida diaper rash – A bright red, bumpy rash in the diaper area caused by yeast overgrowth. It is common in babies and children who wear diapers. The rash has defined edges and may develop satellite lesions.
Yeast infections occur more frequently in those with weakened immune systems or other medical conditions like diabetes. Women are also more prone to vaginal yeast infections during pregnancy while taking antibiotics or birth control pills or when estrogen levels change. Proper diagnosis and treatment can help provide relief from uncomfortable symptoms. OTC topical antifungal creams may be used for mild infections, while more persistent or severe cases may require prescription oral antifungal medication. Practicing good hygiene and wearing breathable fabrics can help prevent recurrence.
How To Cure Fungal Infection On Skin
Fungal skin infections can be treated with over-the-counter (OTC) antifungal creams, oral prescription antifungal medications, and by addressing any predisposing factors.
Some commonly used OTC antifungal creams include:
- Clotrimazole (Lotrimin, Mycelex)
- Miconazole (Monistat, Micatin)
- Terbinafine (Lamisil)
These creams are usually applied to the affected area once or twice a day for 1-2 weeks until symptoms resolve.
For more persistent or widespread infections, oral prescription antifungals may be needed. These include:
- Terbinafine (Lamisil)
- Itraconazole (Sporanox)
- Fluconazole (Diflucan)
Oral antifungals are taken for 2-12 weeks, depending on the type and severity of the infection. Blood tests are sometimes needed to monitor liver function while taking these medications.
Identifying and addressing any predisposing factors contributing to recurrent fungal infections is also important. This includes keeping the skin clean and dry, wearing loose, breathable fabrics, treating conditions like diabetes or immunosuppression, and avoiding prolonged antibiotic use, which can alter normal flora. With proper treatment and preventative measures, fungal skin infections can often be cured and recurrence avoided.
Home Remedies
Several natural antifungal home remedies can help treat fungal skin infections:
-
Tea tree oil contains terpenes-4-ol, which has powerful antifungal properties. Dilute tea tree oil with a carrier oil like coconut oil and apply to affected areas 1-2 times daily.
-
Apple cider vinegar creates an acidic environment that prevents fungus growth. Mix equal vinegar and water and dab onto rashes using a cotton ball.
-
Plain yogurt with live cultures can be applied topically thanks to its probiotics. Apply a thin layer to the affected area and sit for 30 minutes before rinsing.
-
Keeping skin clean and dry can help eliminate excess moisture where fungi thrive. Change socks regularly and wash athletic wear after each use.
-
Wear loose, breathable fabrics like cotton that allow ventilation and moisture evaporation on the skin.
-
After bathing, thoroughly dry the skin, especially between the toes and skin folds where moisture gets trapped.
-
Allow the skin to breathe as much as possible. Go barefoot when at home and avoid tight clothing.
By using natural antifungals and keeping the skin clean, dry, and well-ventilated, home remedies can effectively treat fungal infections while avoiding medication side effects. However, see a doctor if symptoms worsen or don’t improve within 1-2 weeks.
Prevention
The best way to deal with fungal skin infections is to prevent them from occurring in the first place. This involves keeping the skin clean, dry and well-ventilated.
- Wear loose, breathable natural fabrics like cotton that allow skin to breathe. Avoid tight clothing that traps heat and sweat.
- Thoroughly dry the skin after bathing or swimming, especially between the toes and skin folds where moisture gets trapped.
- Dust antifungal powder on the feet, groin, and other prone areas to help keep them dry.
- Treat fungal infections like athlete’s foot promptly. Left untreated, they can spread to other areas of the body.
- Replace old shoes and socks regularly that may harbor fungal spores. Consider wearing flip-flops in public showers or locker rooms.
- Keep toenails trimmed short to avoid cuts that could become infected.
- Avoid sharing towels, clothing, or shoes with others infected.
Good hygiene and prevention habits can reduce the frequency and recurrence of uncomfortable fungal skin rashes. Stopping the problem before it starts is ideal.
When to See a Doctor
Over-the-counter antifungal treatments are effective for most fungal skin infections. However, you may need to see a doctor if:
-
The infection does not improve with OTC antifungal creams after 2 weeks of consistent use. The infection may be resistant to those treatments and require prescription medication.
-
You develop a fever, or the rash is spreading. This could indicate a secondary bacterial infection that requires antibiotics or other treatment.
-
You have other medical conditions like diabetes or a weakened immune system. These increase susceptibility to fungal infections and their complications.
-
The infection is severe, widespread, or in a sensitive area like the groin. A doctor can provide stronger prescription medications.
-
You experience significant pain, swelling, pus, foul odor or other signs the infection is advancing. Aggressive treatment is required.
-
The rash persists despite OTC treatments, and you’re uncertain of the cause. A doctor can perform diagnostic testing to determine if it is a fungal or another skin condition.
See your doctor promptly if your fungal infection is worsening, spreading, or not responding to self-care. They can prescribe more potent antifungal treatments to clear the infection before complications develop.
Conclusion
Fungal skin infections are very common conditions that most people will experience at some point in their lives. The main symptoms are itching, redness, and a rash in moist areas of the body. While uncomfortable, these infections are generally harmless and treatable with over-the-counter antifungal creams, keeping the area clean and dry and preventing recurrence.
However, fungal skin infections return if proper precautions are not taken. This is why prevention is key – wearing breathable fabrics, thoroughly drying the skin, and applying antifungal powder can help stop the proliferation of fungus and avoid repeat infections. Recurring infections that fail to respond to home treatment may require prescription antifungal medicine.
In summary, fungal skin problems can be managed and controlled with diligent hygiene and prompt treatment. But if the infection is severe or keeps returning, it’s best to see a dermatologist for evaluation and prescription-strength medication. Catching and curing fungal infections early is important to prevent their spread to the body. Most people find relief from the irritation of fungal skin infections with proper care.
Jillian Ruffo
As a Beauty Care and Wellness Writer, of liveandfeel I focus on the holistic concept of wellness, encompassing mental, physical, and emotional health. I create engaging content that informs and empowers readers to prioritize self-care. My content celebrates diverse definitions of beauty and encourages self-love. I explore natural ingredients, cutting-edge beauty technologies, and mindfulness practices, fostering a sense of well-rounded well-being. My goal is to inspire readers to prioritize self-care and discover the latest trends in beauty.